Payers
Scaling services to improve outcomes
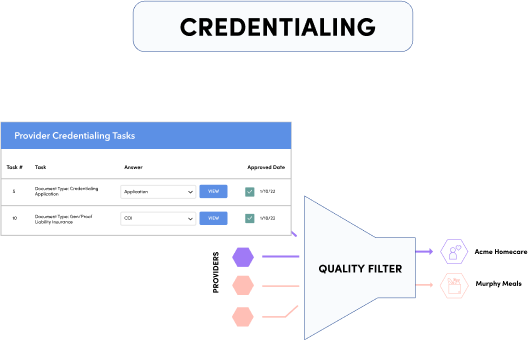
The Helper Bees’ platform enabled the creation of our nationwide Aging-In-Place Provider Network and allows for continuous expansion of in-home service providers that deliver everything from home care to home modifications – and more.
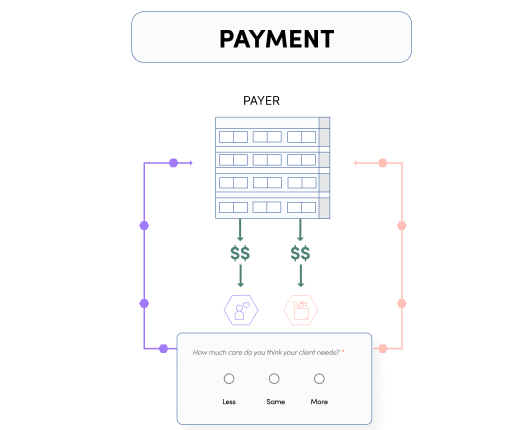
In addition to our network, the platform ensures reliable and scalable service fulfillment, with digital claims tools that simplify the claims process, improve data collection, and help detect fraud using advanced analytics. By providing payers access to the platform, we are able to reduce costs while simultaneously improving health outcomes for older adults.